Right-Sizing Credentialing Software for Rural Hospitals: Stop Buying “Big Health System” Problems

Running a rural hospital is arguably the toughest job in healthcare today. With razor-thin margins and relentless operational pressures, every dollar spent on enterprise software must prove its worth immediately. The hard reality is that administrative bottlenecks in your medical staff office directly translate to delayed billing and crippled cash flow. When CEOs and CFOs evaluate credentialing and payor enrollment software, the stakes could not be higher.
The executives who navigate this successfully understand a fundamental truth: software designed for massive, multi-facility health systems is a trap for rural facilities. Here is how rural leaders can right-size their technology to protect their revenue cycle and eliminate administrative chaos.
The “Big Hospital” Software Trap
The Myth: Buying top-tier, enterprise-level software will naturally modernize and elevate your rural hospital’s operations.
The Reality: Heavy enterprise software is built for scale, complexity, and specialized departments. In a rural or Critical Access Hospital (CAH), the reality is “multiple hats.” The same person managing Primary Source Verification might also be running payroll and handling compliance reporting. Forcing a stretched, overworked team to click through 40 irrelevant screens meant for a sprawling academic medical center causes massive inefficiency and user fatigue.

Executive Action: Shift to OpEx Pricing Models
Mandate a shift toward predictable, per-provider pricing models (OpEx) rather than massive upfront enterprise licenses (CapEx). Choose platforms designed explicitly for the lean, multi-tasking reality of rural healthcare staffing.
Common Buying Mistakes Ruining Your ROI
The Problem: The EHR Bolt-On and Implementation Fatigue
Executives often bundle credentialing software into their massive Electronic Health Record (EHR) purchase, assuming the bolt-on module is “good enough.” Unfortunately, EHR-native credentialing tools are notoriously clunky and frequently lack the crucial payor enrollment connections needed to get your hospital paid faster.
Furthermore, enterprise implementations can take 12 to 24 months, a timeline rural facilities simply cannot afford. If a system requires your small IT team to build custom API bridges, the project will inevitably stall.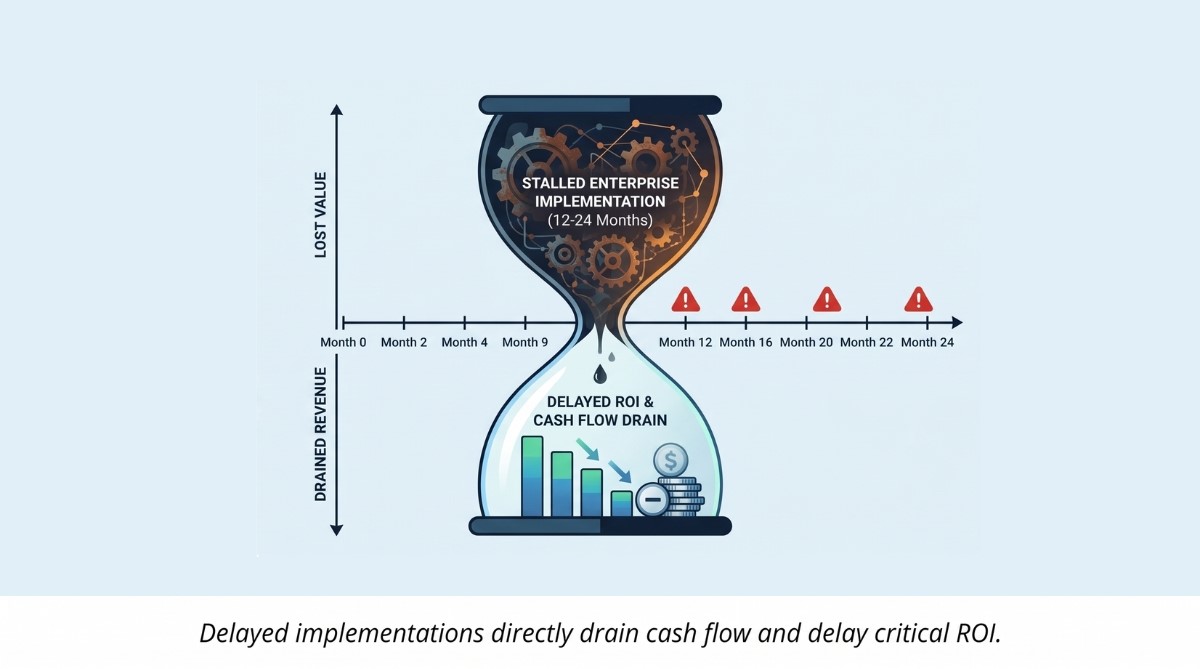
Executive Action: Separate Credentialing from the EHR
Separate your credentialing strategy from your EHR core. Demand a clear timeline to ROI by prioritizing “results-ready” software that guarantees an out-of-the-box implementation in 60 to 90 days.
What to Adapt vs. What to Leave Behind
The Problem: Over-Engineering the Credentialing Process
A CFO might buy a system because the financial modeling looks great, without realizing the software forces the facility into highly complex, customized workflows. Trying to replicate a massive health system’s bespoke matrix privileging inside a 25-bed hospital is a recipe for disaster. If the platform is a nightmare for locum tenens or visiting specialists to use, provider satisfaction plummets and onboarding stalls.
Executive Action: Focus on Core Functions
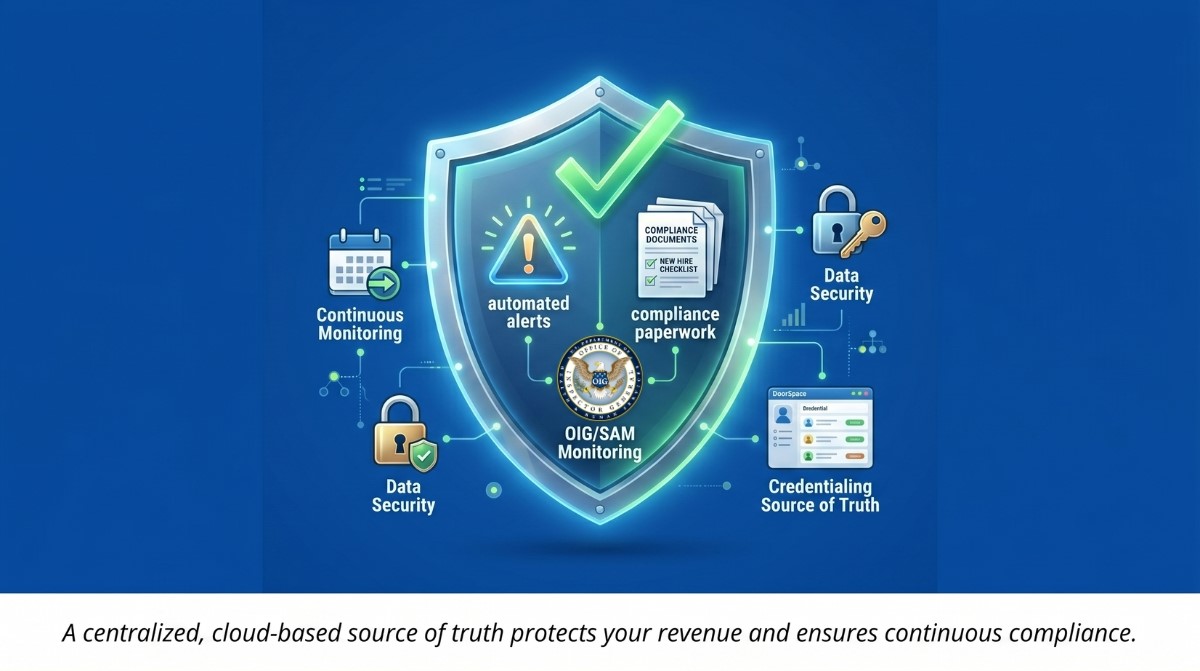
Stop paying for feature bloat and focus on the non-negotiables. You must adapt these three core functions:
- Automated Expiration Alerts: A lapsed credential can sideline a provider for weeks, leading to delayed payments that drag out for 90-180 days. Automated tracking is mandatory.
- Centralized Source of Truth: Moving away from tribal knowledge and filing cabinets to a single cloud-based repository is critical for institutional resilience.
- Continuous Monitoring: Automate your OIG/SAM exclusion checks to maintain seamless Joint Commission (TJC) / CMS compliance without the manual labor.
The Bottom Line: Process First, Technology Second
The biggest mistake a leadership team can make is trying to solve a process problem with technology alone. If your hospital’s credentialing process is deeply broken, chaotic, and heavily reliant on one employee’s memory, expensive software won’t fix it; it will only digitize the chaos.
The best leaders pause to standardize their internal policies first. By adopting right-sized software that forces your team into clean, standardized workflows, you eliminate friction, accelerate your revenue cycle, and empower your staff to focus on what matters most: patient care.
Technology should serve your mission, not add to your administrative burden. If your team is still wrestling with “spreadsheet hell” and fragmented data, it’s time to modernize.
Let’s talk about building a unified digital infrastructure for your rural health system.
